Experts from Centene and UnitedHealth Group on “Making the Case for Enterprise Clinical Data Integration”
January is filled with “Best of 2021” listicles, so we were inspired to check out our Resources and create our own list! We found this excellent AHIP webinar, which first aired in the spring of 2021. It contains wise advice on how health plans can approach clinical data integration at the enterprise level. Our original blog post published after that webinar highlighted key learnings. In this updated post we also guide you to some of the most informative parts of the program.
Terry Boch, Diameter Health’s Chief Commercial Officer, moderated a discussion with Darren Schulte, MD, President of Advanced Technology at Centene Corporation, and Mike Baillie, Senior Vice President of Business Development at UnitedHealth Group.
Darren and Mike shared their experience and insights on three primary topics during the session:
- How to build a winning strategy: top down or bottom up? (Jump in at 10:56 min)
- Common organizational roadblocks and how to overcome them. (28:21 min)
- Key metrics to demonstrate ROI. (45:17 min)
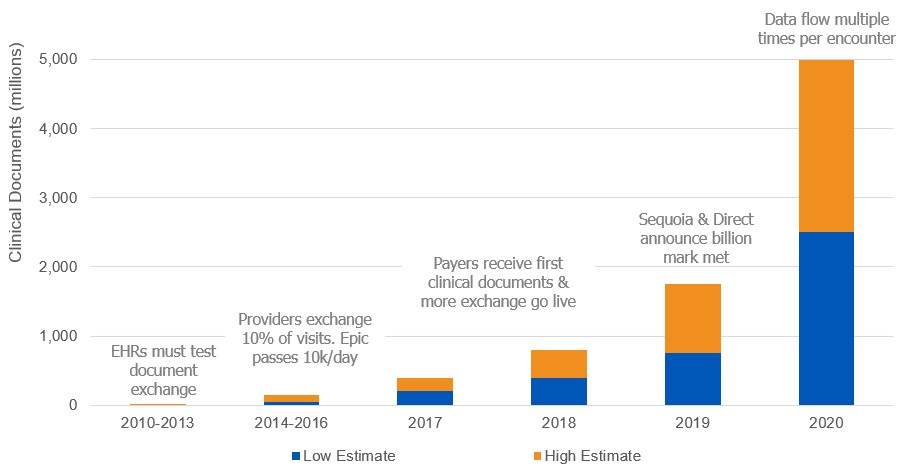
To kick off the webinar, Terry noted that estimates of the total volume of digital clinical data exchanged since 2010 in the US has exploded from near zero into the billions.
“Given what we’re seeing in the industry from a clinical document exchange perspective, data is being shared at unprecedented levels.”
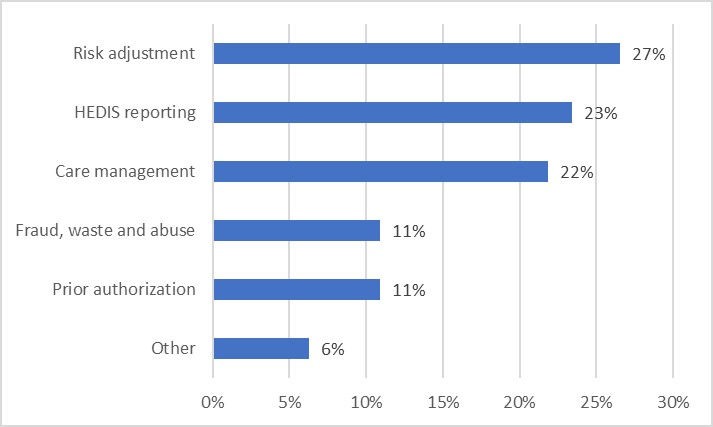
The panelists and the audience identified high-value use cases that form the basis for a business justification for enterprise clinical data integration. Here’s the audience view:
Poll: What use cases are your greatest priorities for using clinical data?
Mike and Darren both underscore the underlying challenge: clinical data integration requires an Enterprise focus justified by the economics of discrete use cases from across the Enterprise. Mike also suggests that shared incentives between Payers and Providers (or “Value-Based Contracting”) will increase clinical data sharing between payers and providers.
“Instead of “value-based care,” I say “value-based contracting.” How do you create agreements with your providers where there are shared incentives around reducing the total cost of care through things like HEDIS and (other) programs… that motivate the provider and payer to bidirectionally exchange data?”
Darren explains his approach to “connect once and use many” by focusing on high-value use cases like Risk Adjustment and HEDIS reporting (the audience agreed; these are also the top two use cases reported in our poll).
“We take this approach where we connect once and use many, many times. But you need that use case that enables you to connect once across the largest array of data sources and that use case will drive the data…that flows through the pipes.”
Darren also walks through the Risk Adjustment use case, and details, for example, cost savings from substituting the use of digital charts for manual chart pulls and improved revenue opportunities in Medicare Advantage programs from more accurate risk adjustment through the use of clinical data.
“ROI follows the business case you’re trying to further using the data strategies and it starts with the baseline… how this data liquidity will enable you to reduce your cost of operations, reduce your cost of care, (and) or improve the care being delivered, as it ties to the use case.”
Poll: What are the greatest obstacles to successfully pursuing an enterprise clinical data strategy?
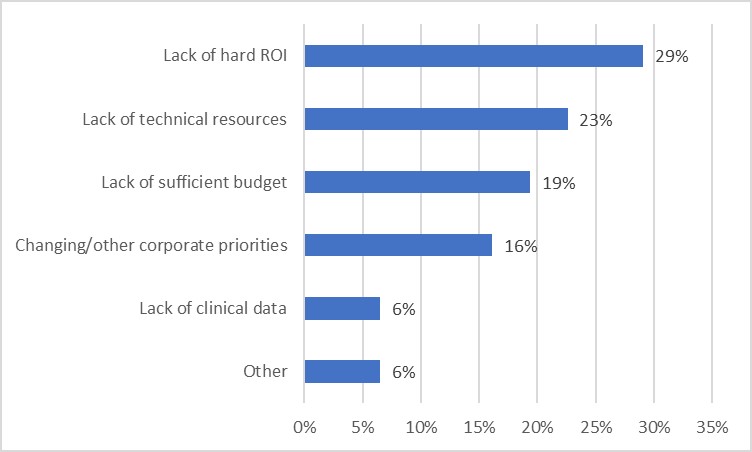
Notice that only a small percentage of those responding cite “lack of clinical data” as a major obstacle to their enterprise data strategy. One conclusion is that when clear ROI is demonstrated, internal resources and other priorities cease to be barriers to success.
Final Insights
UnitedHealth and Centene are in the vanguard of health plans putting clinical data to Enterprise use. The lessons they learned along the way can save others time and money:
- Follow the money. As risk is increasingly shared between payers and providers, incentives will increase for data sharing
“Follow the money. As we shift risk to the provider from a clinical and financial risk standpoint, that enables more of a partnership… and provides the impetus for (a) strategy for integration that doesn’t rely on individual use cases.”
- Take a pragmatic approach. Our panelists agreed that while the industry is advancing toward data standards, that’s not the case today; expect to meet the market where they are
- Expect clinical data quality issues. Raw clinical data is not actionable without refinement
“When you get multi-modal data from various sources, we have to not only normalize the thousand different ways hemoglobin HbA1c is reflected in a data set, but also think about errors, concordance issues… (for example,) diabetes is present, but lab tests and other data don’t indicate as such. There are still a lot of EHR quality issues…”
Thanks again to Darren and Mike for participating with Terry on the panel. We are privileged to work with clients like them who are both knowledgeable and willing to share that knowledge with the community.


